Brachytherapy Prostate Cancer
What Is Brachytherapy For Prostate Cancer
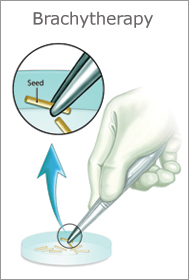 |
| Brachytherapy Prostate Cancer |
Brachytherapy also known as prostate seed implants, is a kind of internal radiation treatment for prostate cancer. Radioactive brachytherapy implant seeds to the prostate cancer.
Brachytherapy prostate cancer requires the use of ultrasound and template guided insertion of radioactive seeds into the gland. The
brachytherapy seeds will wipe out the cancer cells in the prostate.
History of Brachytherapy Prostate Cancer
It was recorded that around the year 1901, not long after the uncovering of radioactivity, Pierre Curie from France is the 1st to suggests the use of radioactive isotopes for treating cancer. Approximately the same time, Alexander Graham Bell of America also suggested it which started the involvement in refining the science within the medical profession. Henri-Alexandre Danlos of the Curie Institute in France and Robert Abbe of St. Luke's Memorial Hospital in New York are 2 initiators of brachytherapy, begin testing the idea of contracting the tumors by exposing it to radioactive materials. These early evolutions offered involvement into the effects of radiotherapy.
In 1970's, numerous medical centers starts to employed brachytherapy to prostate cancer treatment. Radioactive seeds were localised using an unfold operative method, whereby the the operating surgeon would apply a finger positioned in the rectum to distinguish the rough localisation of the tumor and direct the radioactive material accordingly.
Following up of these early cases in the long run often found unsatisfactory results and the cancer control can not be predicted. These results were the consequence of technical unfitness to precisely lay the seeds and lack of decent means to judge the intensity of the prostate gland to formulate an effective dose during that time.
During the late 80's and early 90's the innovation of transrectal ultrasound came forth, providing better evaluation of the prostate. This progression immediately dealt with the demand for better estimation of the prostate volume. With the combination of the template guidance, or precise needle positioning of radioactive seeds, Magnetic Resonance Imaging (MRI) and Computed Tomography (CT) technical advancement the issues of the early years were addressed. Advanced brachytherapy is reckon a viable treatment for prostate cancer.
Types of Brachytherapy for prostate cancer
There are two types of brachytherapy, high dose rate (hdr) brachytherapy prostate cancer and low dose rate (ldr) brachytherapy prostate cancer.
Low dose brachytherapy prostate cancer is more commonly used. During the process, brachytherapy seeds are implanted into the prostate cancer using a ultrasound guidance. The number of brachytherapy seeds and their placements are dictated by a computer generated therapy plan for individual patient. The seeds are place permanently in the prostate until it become expire after a few months.
High dose rate brachytherapy for prostate cancer is a newer therapy and requires the impermanent arrangement of hollow needles in the prostate. They are filled with a radioactive substance for few minutes and then extracted. This is replicated 2 to 3 more times over a period of several days.
Brachytherapy For Prostate Cancer Criteria
Brachytherapy may be an option for patients with lower Gleason score, lower PSA level and a tumour that has not outspread to other area of the body. If there is a higher likeliness that the prostate cancer may have spread to the surrounding tissues of the prostate, patients may be offered a short course of external beam radiotherapy before going through a brachytherapy implant. This combining therapy provides a more allowance to treat the tissue around the prostate.
Brachytherapy For Prostate Cancer Procedure
Brachytherapy prostate cancer is carried out in two stages:
Stage 1, is the volume study. A catheter is temporarily inserted into paient's urethra during the volume study under anaesthetic condition. This is to identify the structure. There might be slight discomfort during the first urination after the brachytherapy prostate cancer procedure.
Stage 2, is the implantation process of the brachytherapy seeds. The procedure is also executed under anaesthetic condition. Brachytherapy seeds are introduced under transrectal ultrasound guidance, using needles that go through through the skin of the perineum which is behind the scrotum. Each needle may render 2 to 6 seeds and, usually, 20 to 30 needles are necessary to have 80 to120 seeds implanted. Majority of the seeds inserted are woven into a filament of absorbable material to aid in preserving their position and will remain permanently in place.
A catheter is once again inserted into the urethra under anaesthetic condition which will remain for a few hours after the procedure. X-rays are filmed throughout the brachytherapy prostate cancer procedure, to ascertain the position of the brachytherapy seeds.
Brachytherapy For Prostate cancer Precautions
Specific precautions is necessary where the patient's partner is pregnant at the time of implantation. The followings are general recommendations for the first two months after Brachytherapy seed implantation:
- To avoid sex for the 1st two weeks
- Subsequently after the 1st two weeks, advise to use a condom during sex to prevent the seed from passing during ejaculation
- Avoid close contact with pregnant women and children.
- Avoid children to sit on lap for long periods of time
- If travelling to other countries is unavoidable, consider carrying a mediacal card to indicates that you have had a prostate seed implant in case of any radiation detectors encounter at checkpoints. .
Tags:
Brachytherapy Prostate Cancer
What Is Brachytherapy For Prostate Cancer
History of Brachytherapy Prostate Cancer
Types of Brachytherapy for prostate cancer
Brachytherapy For Prostate Cancer Criteria
Brachytherapy For Prostate Cancer Procedure
Brachytherapy For Prostate cancer Precautions
Brachytherapy For Stage 3 Prostate Cancer
Brachytherapy For
Prostate Cancer Young Men
Best Brachytherapy Prostate Cancer
Brachytherapy Cured My Prostate Cancer
Define Brachytherapy Prostate Cancer
Brachytherapy Localised Prostate Cancer
Brachytherapy Implant Prostate Cancer
Brachytherapy For Localized Prostate Cancer
Brachytherapy For Clinically Localized Prostate Cancer Optimal Patient Selection
Brachytherapy Metastatic Prostate Cancer
Brachytherapy Of Prostate Cancer
Prostate Cancer Treatment Options Brachytherapy
Brachytherapy For Prostate Cancer Pdf
Treating Prostate Cancer With Brachytherapy
Brachytherapy Stage 4 Prostate Cancer
Brachytherapy Seeds For Prostate Cancer
Brachytherapy Seeds Prostate Cancer
High Dose Rate Brachytherapy Prostate Cancer
High Dose Brachytherapy For Prostate Cancer
Hdr Brachytherapy Prostate Cancer
High-dose Rate Brachytherapy Prostate Cancer
High Dose Brachytherapy Prostate Cancer
Low Dose Brachytherapy Prostate Cancer
Low Dose Rate Brachytherapy Prostate Cancer
Ldr Brachytherapy Prostate Cancer
Hdr Brachytherapy Procedure Prostate Cancer







